
How HeartLink Works
Heart failure is dynamic, and meaningful change is not always immediately apparent
HeartLink uses a baseline-relative approach to surface meaningful patient change over time while reducing unnecessary noise. By interpreting daily patient check-ins in longitudinal context—relative to each individual’s own baseline—HeartLink helps outpatient heart failure teams prioritize clinical review without relying on static thresholds or generating unnecessary alerts.

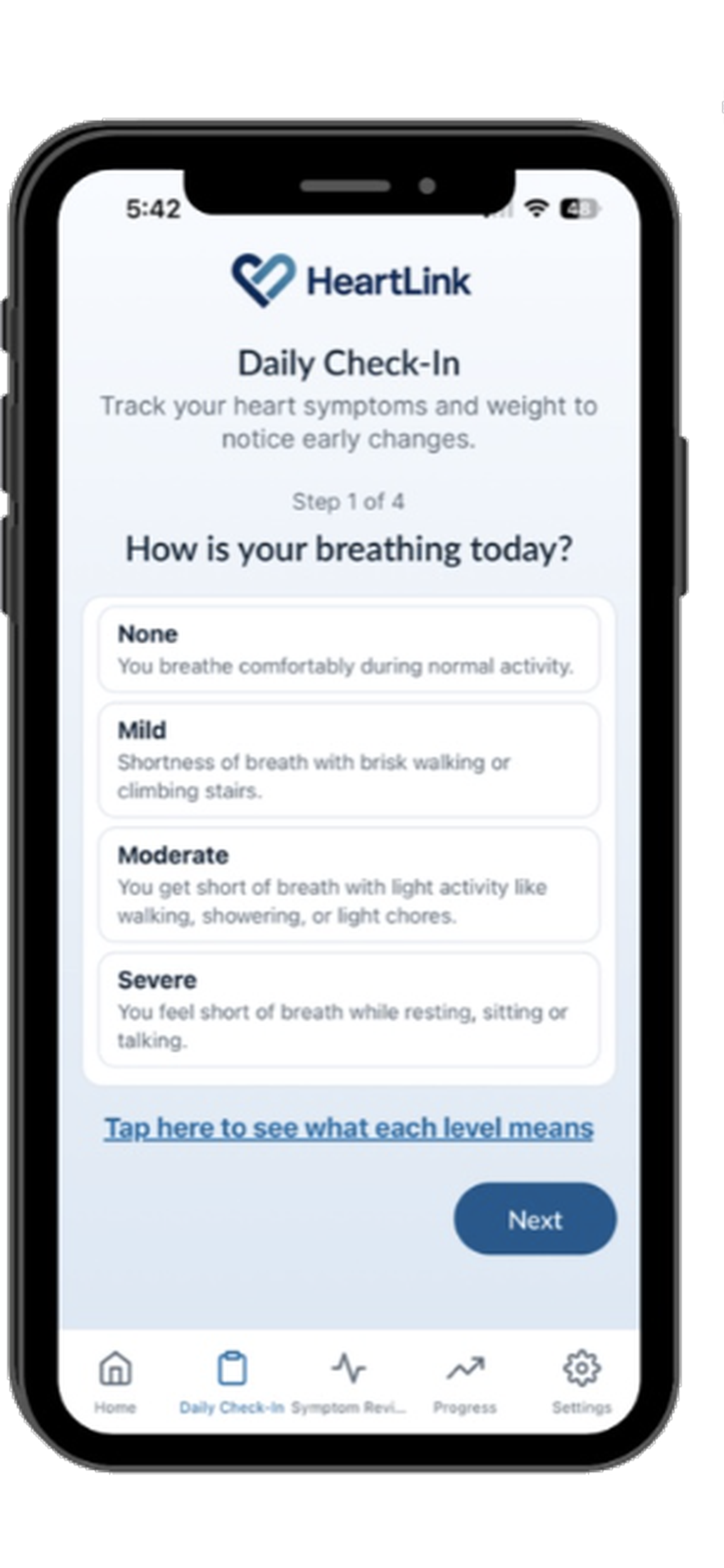
Simple Daily Check-Ins Designed for Consistency
Patients share brief daily updates using the same core symptom domains
Each day patients complete a short check-in focused on how they are feeling relative to their usual state. The experience is intentionally lightweight and familiar, supporting long-term participation without burden.
Daily check-ins include
Shortness of breath
Swelling (edema)
Fatigue
Orthopnea
Weight (when available)
Heart rate and blood pressure logging
What patients do not receive:
No alerts or alarms
No diagnoses
No treatment recommendations
No pressure to interpret medical meaning
HeartLink supports awareness, it does not replace clinical guidance.
A Living Baseline — Interpreting Change Over Time
HeartLink evaluates patient change in longitudinal context, relative to who the patient is now—not a fixed point in the past.
When patients enroll, they complete a baseline describing their usual symptoms. This initial baseline establishes a foundation for understanding each patient’s typical state—but it is not treated as a permanent reference.
Over time, HeartLink carefully evaluates whether a more recent and stable pattern of symptoms should become the active baseline. This process is intentionally conservative and safety-bounded, allowing gradual clinical change to be recognized without overreacting to short-term variability, recovery periods, or expected fluctuation.
Daily patient check-ins are interpreted against the most appropriate baseline—either the original foundation or a qualified updated baseline—along with recent symptom patterns and longer-term trends. Rather than reacting to isolated data points, HeartLink looks for meaningful deviation over time so changes are interpreted in the correct clinical context.
Designed to reduce false escalation
HeartLink applies conservative guardrails so that single-day changes, expected fluctuations, or transient symptoms do not create unnecessary urgency. Interpretation occurs continuously in the background and is designed to support clinician review—not trigger alerts or automated actions.


HeartLink summarizes baseline-relative insight into four stability categories designed to support review—not replace clinical judgement
Clear Stability Categories for Clinical Prioritization
After interpreting daily check-ins in context, HeartLink summarizes each patient’s current status using one of four stability categories. These categories reflect patters over time, not single data points, and are intended to help clinicians quickly understand where attention may be needed

What these categories do—and do not mean
These categories are designed to support prioritization and situational awareness. They do not diagnose conditions, prescribe actions, or replace clinical decision-making
Different Information for Patients and Clinicians
HeartLink intentionally separates patient-facing feedback from clinician-facing insight to support clarity, safety, and trust
HeartLink is designed for two audiences with different needs. patietns receive simple, supportive feedback focused on awareness and consistency. Clinicians receive structured, comparative insight designed to support review and prioritization. This separation is intentional and foundational to how the platform works.

Why this matters:
By separating patient feedback from clinician insight, HeartLink avoids confusion, reduces anxiety, and preserves clinical judgment—while enabling timely review when meaningful change occurs

HeartLink gives clinicians a calm, organized view of patient stability—supporting prioritization without constant interruptions.
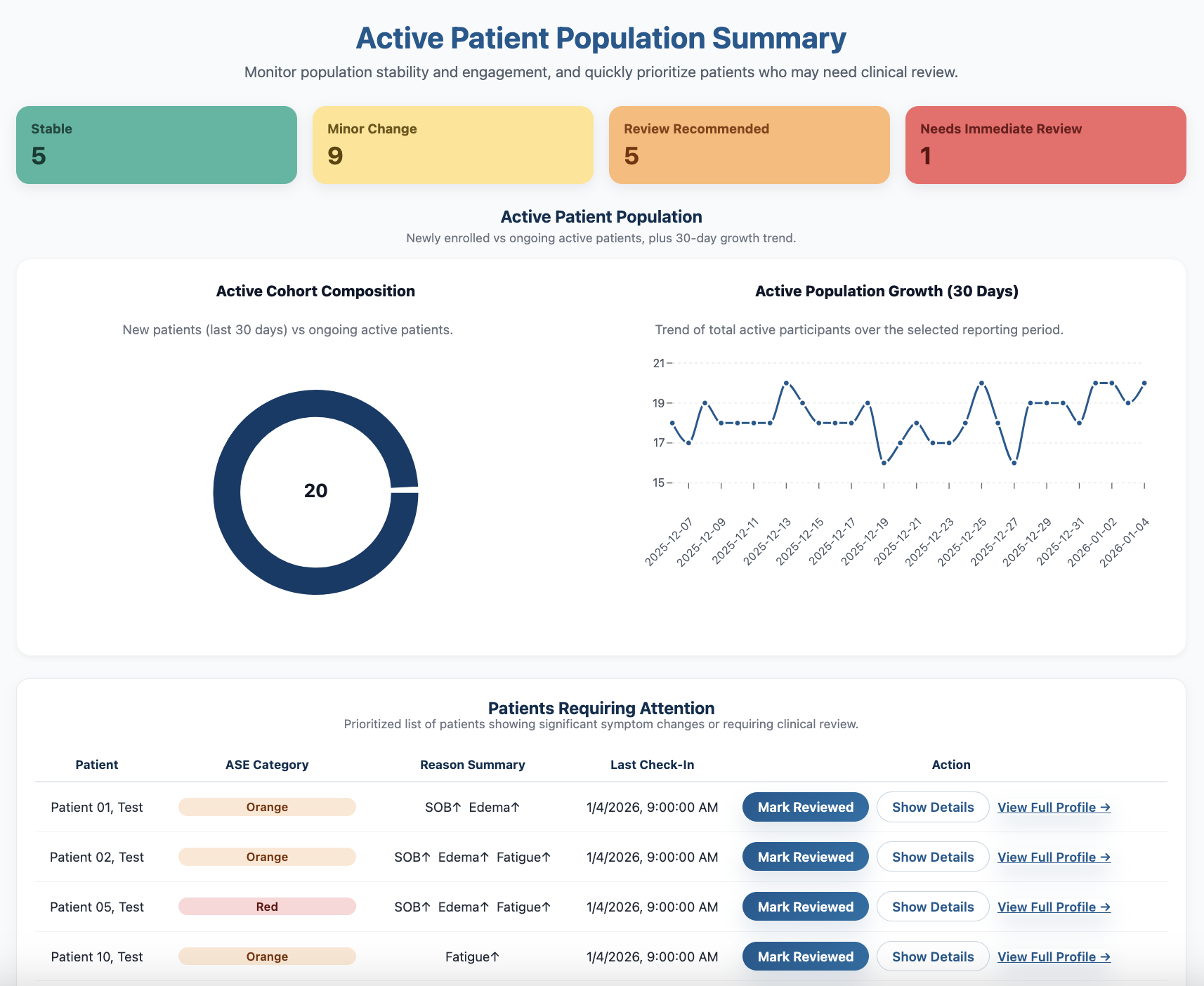
Clear Population Insight for Focused Review
Clinicians begin with a population-level snapshot that summarizes overall stability, engagement, and distribution across the four categories. This view makes it easy to understand how a program is performing at a glance.
From there, clinician can review patients by stability category, identify those who may need attention, and drill into individual detail views when appropriate. Review cadence is intentional and clinician-directed.
Designed for review, not interruption
HeartLink avoids alert-driven workflows. Clinicians decide when and how to review information based on context, capacity, and clinical judgement.
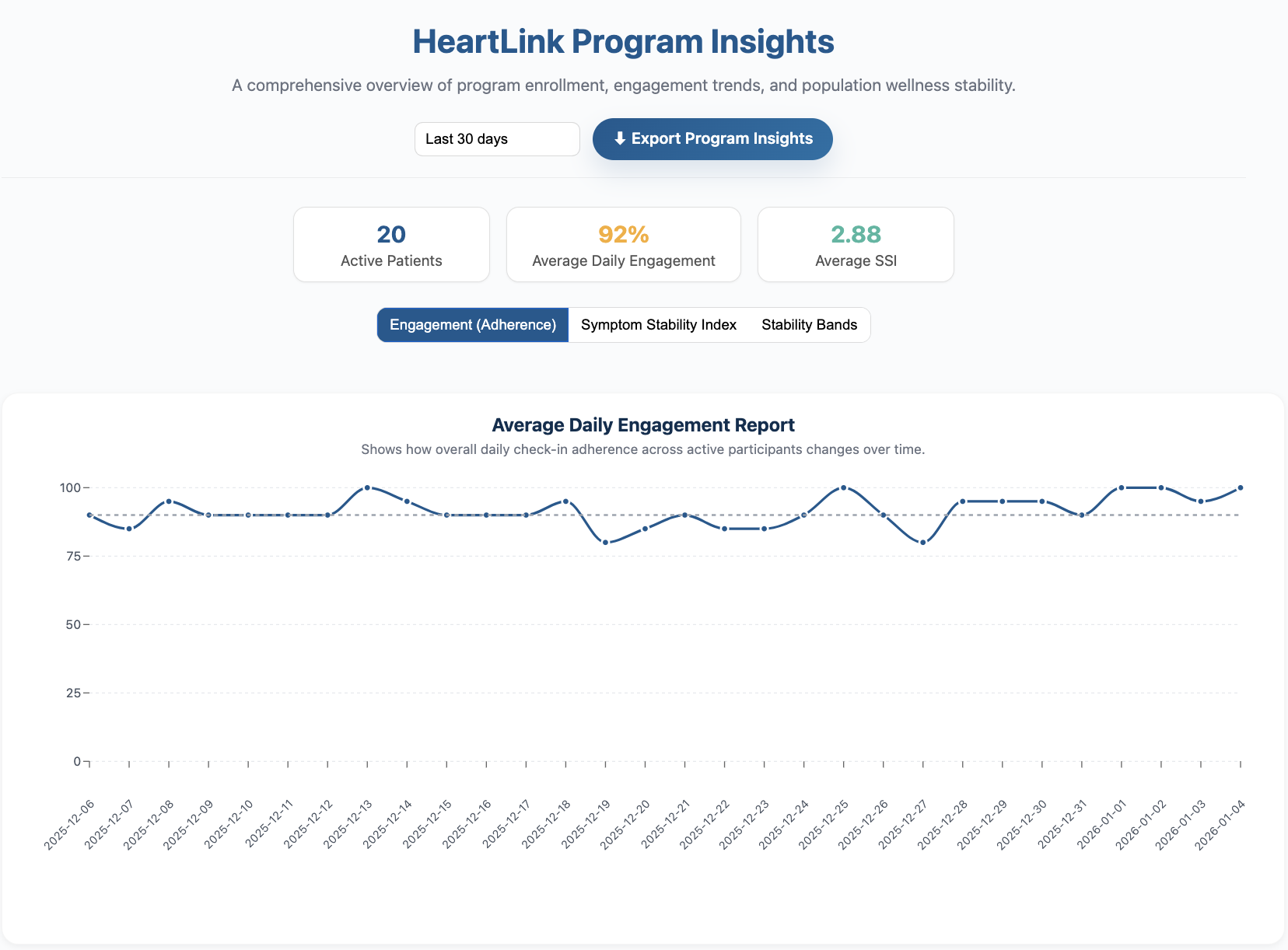
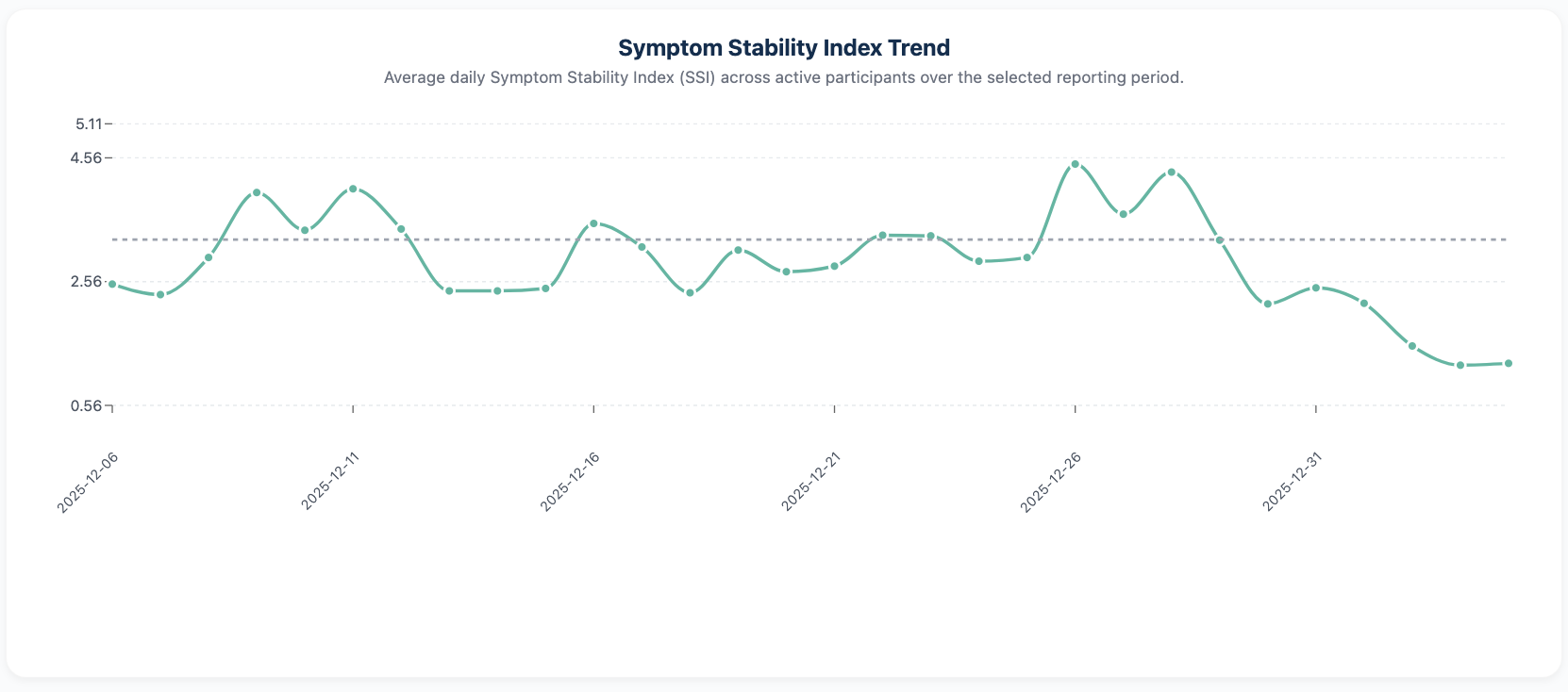
Program-Level Insight Without Data Overload
HeartLink aggregates patient information into clear summaries that support oversight, planning, and quality conversations.
Beyond individual patient review, HeartLink provides program-level views that help teams understand overall engagement, stability distribution, and trends over time.
These summaries are designed to answer practical questions—such as how many patients are stable, how engagement is trending, and whether overall symptom stability is improving—without requiring manual analysis or custom reporting.
Program insights are available directly within the platform and can be exported for internal review or leadership discussions.
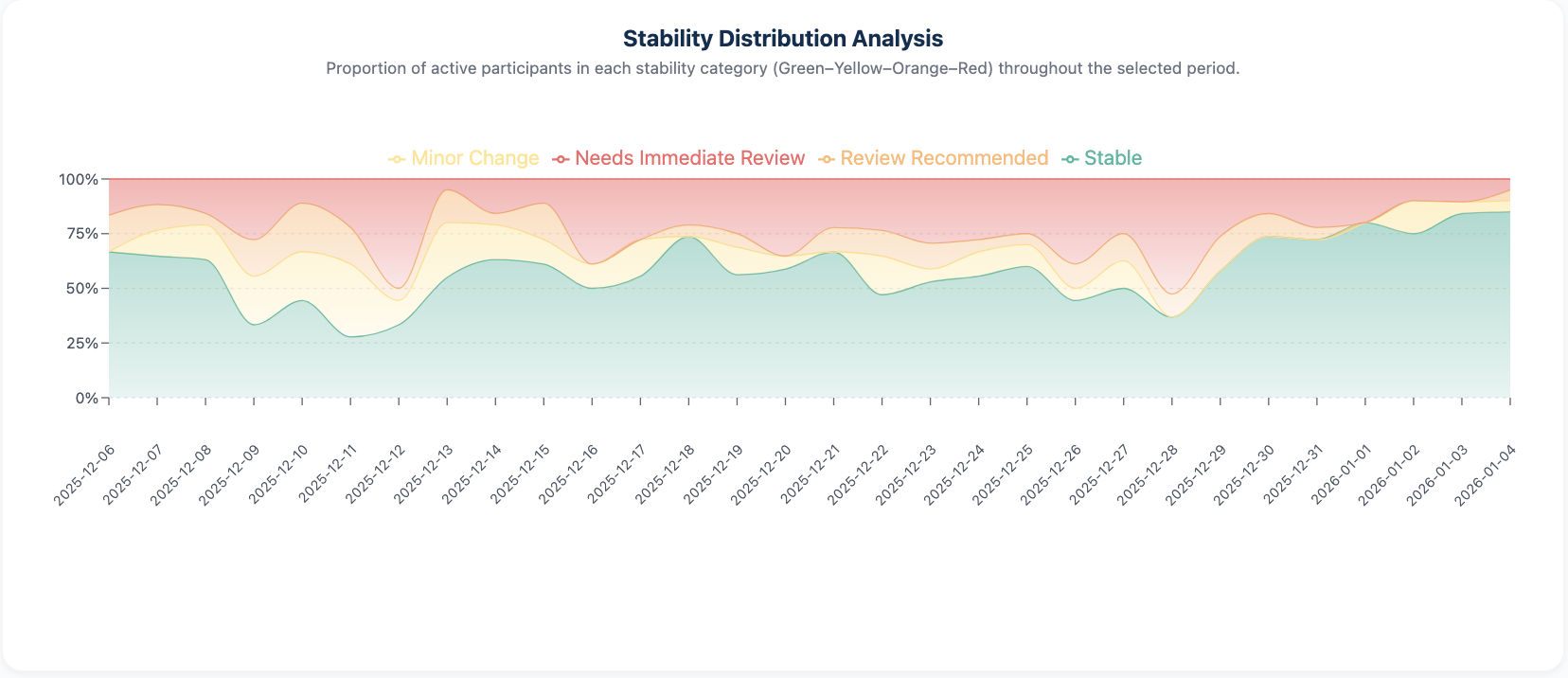
Built for clinical oversight, not automated enforcement
HeartLink provides continuous, program-level visibility to support responsible clinical oversight. Insights are designed to help teams recognize patterns, allocate attention, and guide informed review—without automated actions, performance scoring, or prescriptive decision-making.
